uSBC News & Blogs
2023 archives
December
- 12/4/2023: usbc stakeholder listening sessions: share your vision for achieving infant nutrition security
- 11/29/2023: USBC Membership meeting mission moment with dr. scott hartman
- 11/22/2023: Reflections on Native American Heritage Month: a Conversation with kimberly moore-salas
- 11/21/2023: 2023 Impact Report: breastfeeding policy priorities
- 11/17/2023: USBC Interim EXECUTIVE DIRECTOR ANNOUNCEMENT
- 10/30/2023: USBC Executive director transition announcement
- 9/28/2023: using data to inform infant and young child feeding in emergency preparedness systems
- 9/20/2023: Reviving identity caucuses at the usbc: we want to hear from you!
- 9/19/2023: Reflecting on national breastfeeding month 2023 wins
- 7/28/2023: Fy24 appropriations: what the house and senate bills mean for infant feeding
- 7/25/2023: taking the time for celebration: the pump act and pwfa are law!
- 7/21/2023: news from the chair: change is good
- 3/23/2023: fiscal year 2024 president's budget: what it means for the lactation field
- 3/1/2023: renewing the usbc commitment to equity as we seek to grow the usbc membership network
2022 archives
december
- 12/24/2022: pump for nursing mothers act will soon be signed into law
- 12/8/2022: usda proposes new wic package
- 10/27/2022: 2022 impact report: breastfeeding policy priorities
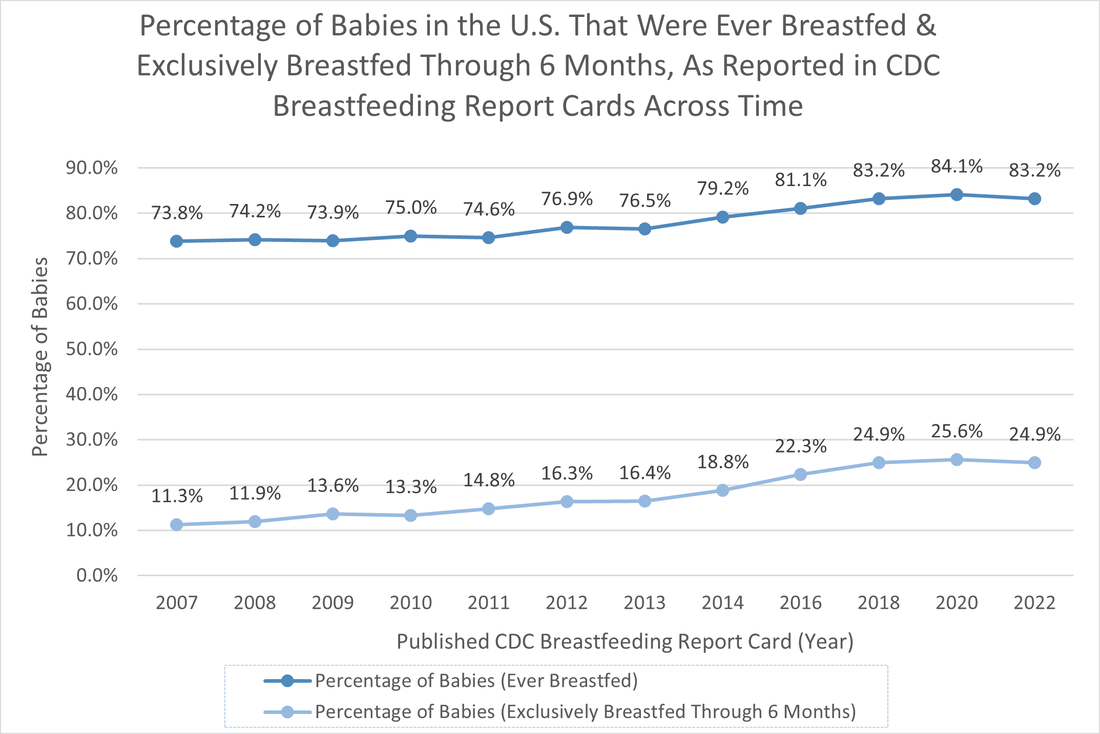
- 10/24/2022: a closer look at the 2022 cdc breastfeeding report card
- 8/24/2022: fy23 appropriations: what the senate bills mean for infant feeding
- 8/18/2022: a consideration of choice (in the absence of systemic supports)*
- 6/24/2022: the senate failed to pass the pump act on wednesday. that hurts. but it doesn't mean the fight is over.
- 6/2/2022: the four pillars of infant nutrition security in the united states
2021 archives
DECEMBER
- 12/9/2021: 2020 state and territory breastfeeding reports now available!
- 12/3/2021: join usbc on our equity journey
- 11/12/2021: 2020 usbc annual report released!
- 10/22/2021: protecting parents, babies, public health, employers, and the economy: a bipartisan case for the pump for nursing mothers act
- 10/22/2021: pump for nursing mothers act passes with bipartisan support in u.s. house of representatives
- 10/20/2021: breaking news: the pump act is going to the house floor for a vote this friday
- 9/30/2021: reflections on national preparedness month and the pandemic
- 9/28/2021: join the nationwide pump act call-in day
- 9/27/2021: the house is voting on the pump act this week. join the week of action.
- 9/26/2021: pump act week of action partner toolkit
- 9/10/2021: reflections on national breastfeeding month 2021: every step of the way
- 8/24/2021: 8 questions answered by the usbc policy team
- 7/29/2021: Cdc awards usbc a five-year grant to coordinate a national approach to improve the infant feeding landscape
- 7/22/2021: fiscal year 2022 house agriculture and dhs appropriations reports released
- 7/16/2021: fiscal year 2022 house labor-hhs appropriations report released
2020 archives


 RSS Feed
RSS Feed
